
You’re in a meeting, trying to stay focused, and it happens again. That small, annoying throat clear that feels impossible to hold back. Or maybe it’s after dinner, when you’re relaxing, and you keep swallowing like something’s stuck. Bedtime can be the worst; the moment you lie down, the tickle starts.
Most of the time, this points to post-nasal drip, which is simply extra mucus sliding from your nose or sinuses down the back of your throat. Your throat doesn’t like that. The lining gets irritated, nerves fire off a “clear it out” signal, and you end up coughing, swallowing, or clearing your throat on repeat.
The good news is that this is common and usually fixable once you identify what’s causing the extra mucus or irritation. The main buckets are nose and sinus triggers, reflux, irritants, and a few practical steps that can calm things down fast.
What post-nasal drip feels like, and why it makes you clear your throat so often
Mucus isn’t the enemy. Your nose and sinuses work all day to trap dust, germs, and allergens. The trouble starts when you make too much mucus, or it gets thicker and doesn’t move well. Then it lingers, and you feel it.
Think of it like a slow leak behind a wall. You might not see water dripping, but you notice the damp feeling. With post-nasal drip, the “leak” is behind your nose, and the sensation shows up as throat irritation.
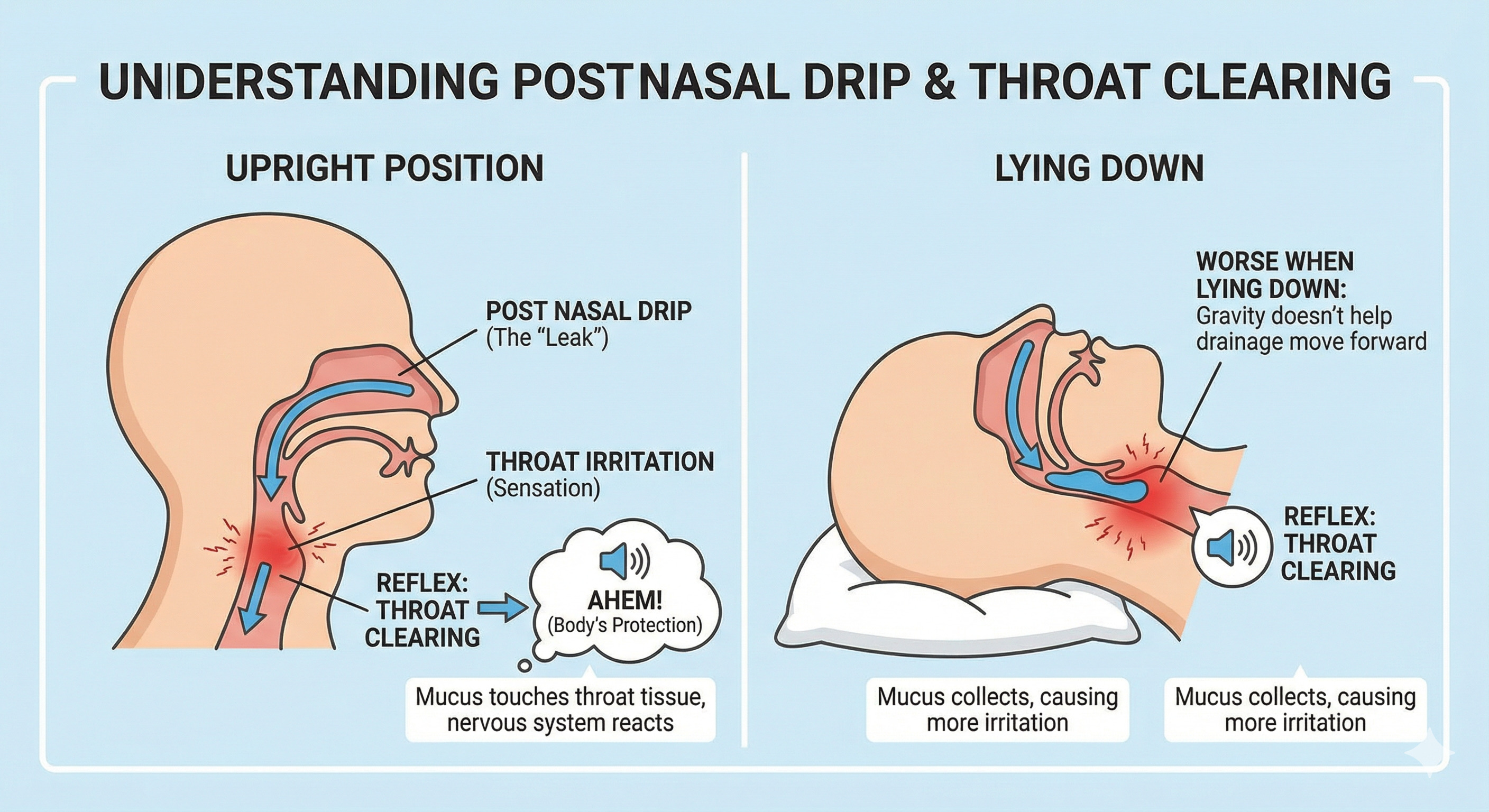
Throat clearing is your body’s reflex. Mucus touches the back of the throat, the tissue gets sensitive, and your nervous system tries to protect your airway. This tends to be worse when you’re lying down, because gravity isn’t helping drainage move forward and out.
Common signs people notice (beyond a runny nose)
Postnasal drip doesn’t always look like a classic “runny nose.” It often feels like throat symptoms first, such as
- A lump or “stuck” feeling in the throat
- Frequent swallowing (even when you aren’t eating)
- A scratchy or irritated throat
- A nagging cough that’s worse at night
- Hoarseness or a voice that tires easily
- Bad breath (from mouth breathing or mucus)
- Mild nausea (mucus can upset the stomach)
- Ear pressure or popping (shared drainage pathways)
These symptoms can be mild but relentless, and they overlap with other issues, which is why cause-finding matters.
Post-nasal drip vs a sore throat or a chest cough: how to tell the difference
Clues usually come from where you feel it and when it shows up. This quick comparison can help:
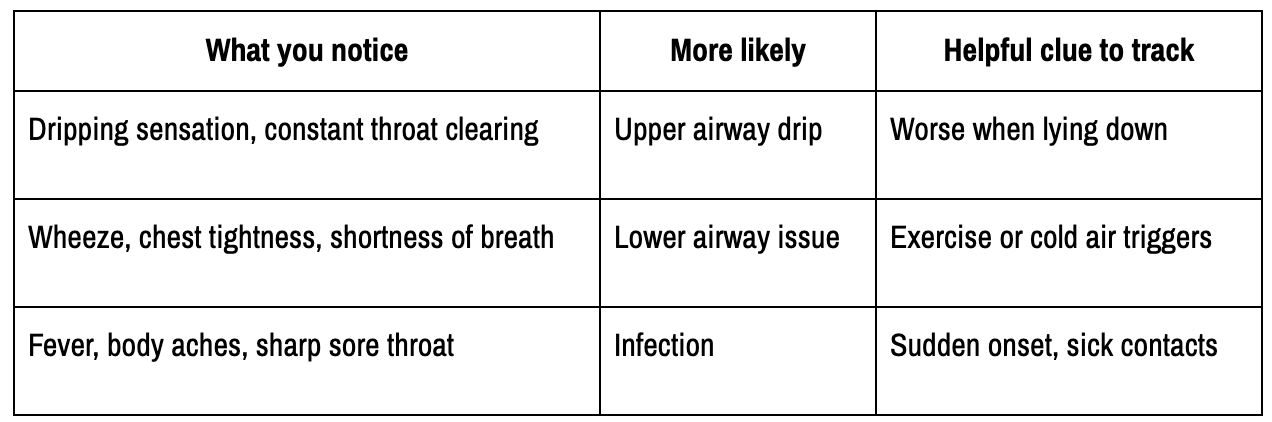

Also, pay attention to timing. Nighttime symptoms, symptoms after meals, and seasonal flare-ups each point in different directions.
The most common causes of post-nasal drip (and the clues that point to each one)
Post-nasal drip often has one main driver, but causes can stack. A simple example is allergies plus dry winter air. You get inflammation from the allergen, then thicker mucus because the air is dry, and now the drip feels nonstop.
If you want a clinician-reviewed summary of symptoms and treatment options, the JAMA Patient Page on postnasal drip is a helpful overview.
Allergies and irritants, the usual suspects
Allergies inflame the lining of the nose. When that tissue swells, it makes more mucus and drains poorly. Common triggers include pollen, dust mites, pet dander, and mold. Irritants act similarly, even without a true allergy, such as smoke, strong fragrances, cleaning chemicals, cold air, and weather shifts.
Clues that fit allergies or irritants:
- Itchy eyes or sneezing
- Clear, watery mucus
- Seasonal patterns, or worse, in specific places (home, work, around pets)
Colds and sinus infections, when thick mucus changes everything
A viral cold can cause post-nasal drip for days, sometimes longer than you expect. Sinusitis can follow, especially if the sinus openings stay swollen and trapped.
Clues that fit a cold or sinusitis:
- Mucus gets thicker and yellow, or green (color alone doesn’t prove bacteria)
- Facial pressure, tooth pressure, or a heavy head feeling
- Reduced sense of smell
- Symptoms that last longer than about 10 days, or improve then worsen again
Antibiotics only help some bacterial cases, so it’s best to let a clinician decide when they’re warranted.
Silent reflux (GERD or LPR), when the problem is coming from below
Sometimes the throat is irritated not by drainage from above, but by reflux from below. With laryngopharyngeal reflux (LPR), stomach contents can reach the throat and voice box. You might not feel classic heartburn, but your throat still reacts with mucus and frequent clearing.
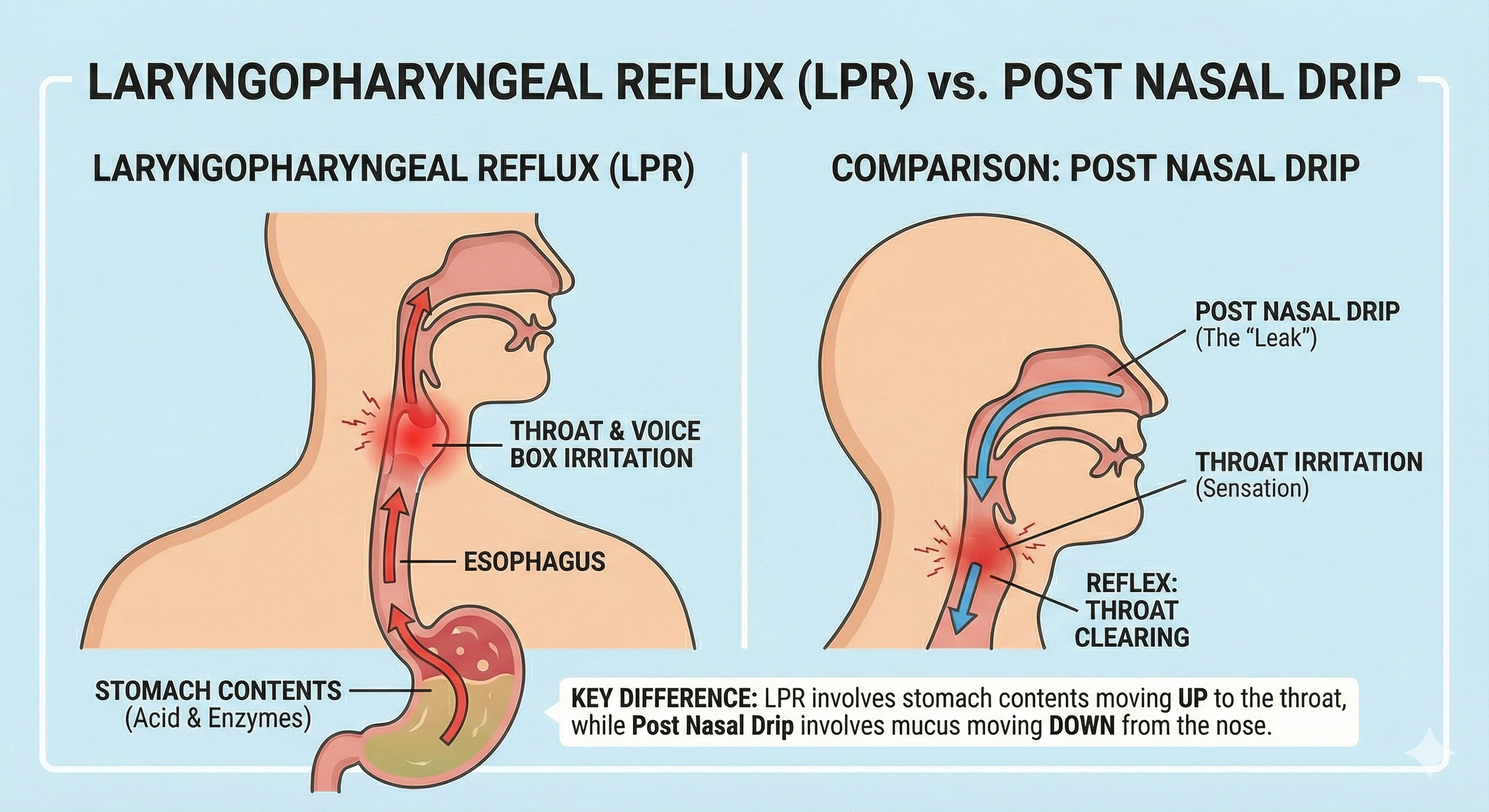
Clues that fit reflux:
- Worse after meals, coffee, chocolate, peppermint, or spicy foods
- Worse when lying down
- Morning hoarseness, a sour taste, or a feeling of throat tightness
Structural and medication-related causes that are easy to overlook
A deviated septum or chronic nasal congestion can change airflow and drainage, which can keep mucus hanging around. Hormonal shifts (including pregnancy) can also increase congestion. Some meds can dry mucus out or irritate the nose.
Don’t stop prescriptions on your own. Instead, review your medication list with a clinician and ask if any might be contributing.
What actually helps, simple steps first, then targeted treatment
The most reliable plan is stepwise: thin and soothe the mucus, calm inflammation, then treat the root cause.
For an evidence-based treatment overview, see Harvard Health’s guide to post-nasal drip treatments.
At-home relief that supports your nose and throat
Start with the basics that make mucus easier to move:
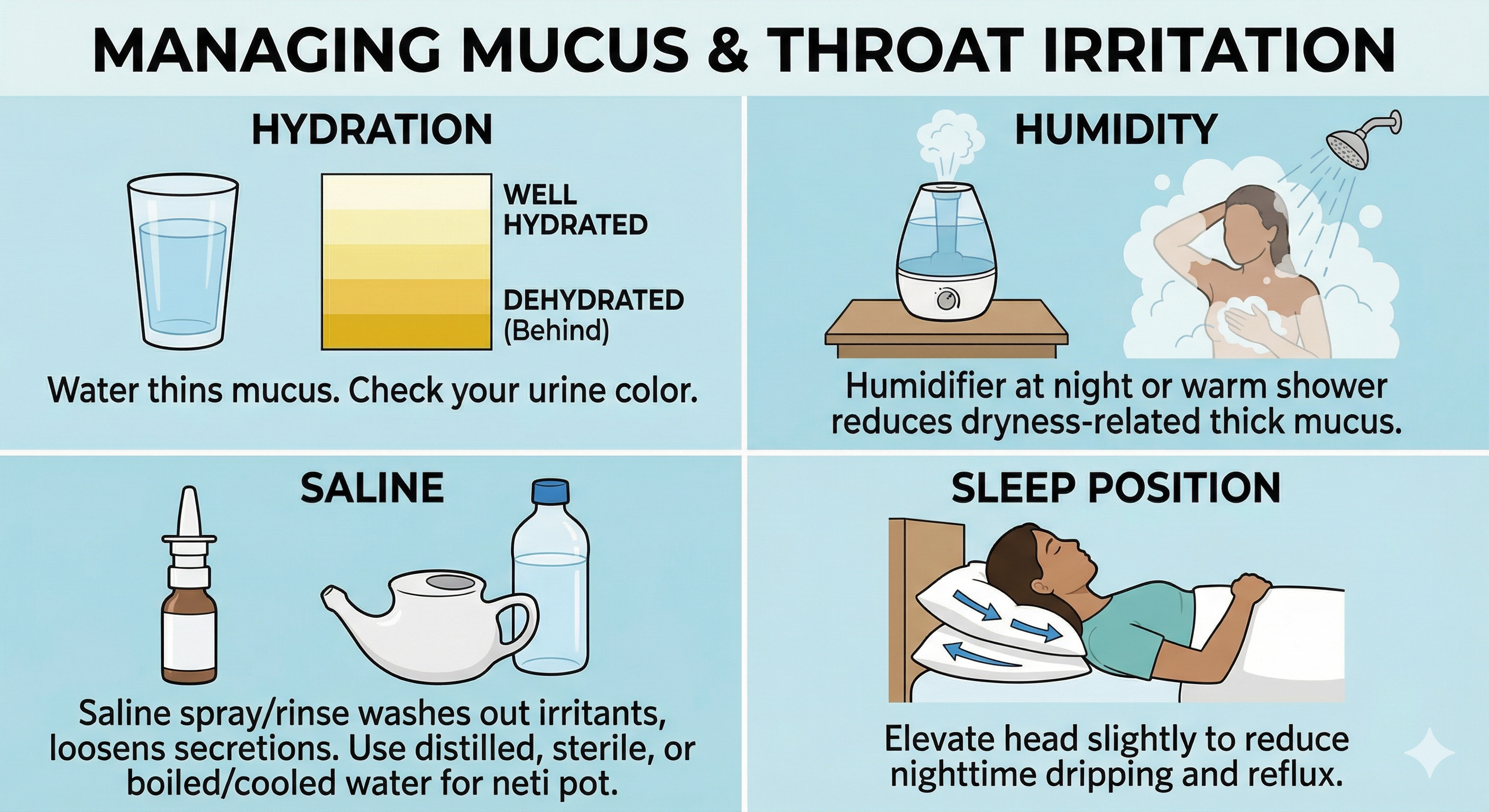
A simple routine that’s easy to follow:
- Morning: saline spray or rinse, then water with breakfast
- Afternoon: a quick check, are you mouth breathing or feeling dry? drink water
- Evening: humidifier, and keep your head a bit elevated
When medicines and testing make sense (and what they are trying to do)
Medication choice depends on the pattern you see.
- Antihistamines can help allergy-driven drip, especially with itching and sneezing.
- Nasal steroid sprays calm swelling inside the nose and can reduce mucus over time. Consistent use matters.
- Decongestants can reduce severe stuffiness short-term, but they’re not for everyone. If you have high blood pressure, glaucoma, are pregnant, or take multiple meds, check with a clinician first.
- Reflux strategies include avoiding meals within 3 hours of bedtime, reducing trigger foods, and using antacids or acid-suppressing meds if advised.
If symptoms keep coming back, allergy testing (skin or blood) can identify triggers and guide treatment. This can be discussed during a virtual visit, including through telehealth medical consultations with Dr. Deepa Grandon.
One more note from recent ENT trends: for stubborn chronic runny nose (chronic rhinitis) that doesn’t respond to usual care, some clinics offer in-office procedures that target overactive nasal nerves. These aren’t first-line, but they can be worth asking about if you’ve tried the basics and you’re still stuck.
A simple 7-day self-check to uncover your trigger
You don’t need a perfect diary, just a quick daily note (30 seconds). Track symptoms and test one change at a time:
- Sleep: flat vs head elevated
- Meals: any food within 3 hours of bedtime
- Exposure: pets, dust, outdoor pollen, strong smells
- Hydration: “low, medium, high” is enough
At the end of 7 days, look for patterns: “worse after late meals,” “worse at home,” or “only at night.” Bringing that log to a visit often speeds up answers.
When throat clearing is a sign to get checked (and what a clinician looks for)
Most throat clearing from post-nasal drip isn’t dangerous, but persistent symptoms deserve a plan, especially if sleep or your voice is taking a hit.
In a visit, a clinician usually focuses on pattern questions (seasonal, after meals, nighttime), checks the nose and throat, and considers allergies, reflux, and infection. Telehealth can be a strong starting point when symptoms are pattern-based and recurring.
Reasons to seek care sooner
Reach out sooner if you notice:
- Symptoms lasting more than 10 days without improvement
- Symptoms that are worsening after initial improvement
- Fever or significant facial pain
- Blood in mucus
- Trouble breathing, chest pain, or persistent wheezing
- Unexplained weight loss
- Severe nighttime cough that disrupts sleep
- Repeated bouts that keep returning
Key Takeaways
Post-nasal drip is one of the most common reasons people keep clearing their throats, and it often comes down to allergies, infection, reflux, irritants, or nasal structure. Start simple: saline, hydration, a little humidity, and a better sleep position. Then use a short symptom log to spot patterns. If it’s persistent or affecting your sleep, voice, or daily life, getting a clear medical plan can turn a nagging symptom into a solved problem.
Stay connected with news and updates!
Join our mailing list to receive the latest news and updates from our team.
Don't worry, your information will not be shared.
We hate SPAM. We will never sell your information, for any reason.
