
“I think I’m allergic to that” is a common reaction after a bad food experience, but it is often incorrect. Reactions to food can come from the immune system, the digestive system, or conditions like celiac disease.
Understanding the difference matters because food allergies can become life-threatening quickly, while most intolerances are uncomfortable but not dangerous.
What a Food Allergy Really Is
In clinical practice, one of the most common issues I see is patients mislabeling intolerance symptoms as allergies, which can lead to unnecessary food restriction or missed diagnosis. A food allergy happens when the immune system treats a food like a threat. In classic IgE-mediated allergies, the body makes antibodies that can trigger mast cells to release chemicals such as histamine. That is why symptoms may hit within minutes. Non-IgE reactions can take longer, but they still involve the immune system.
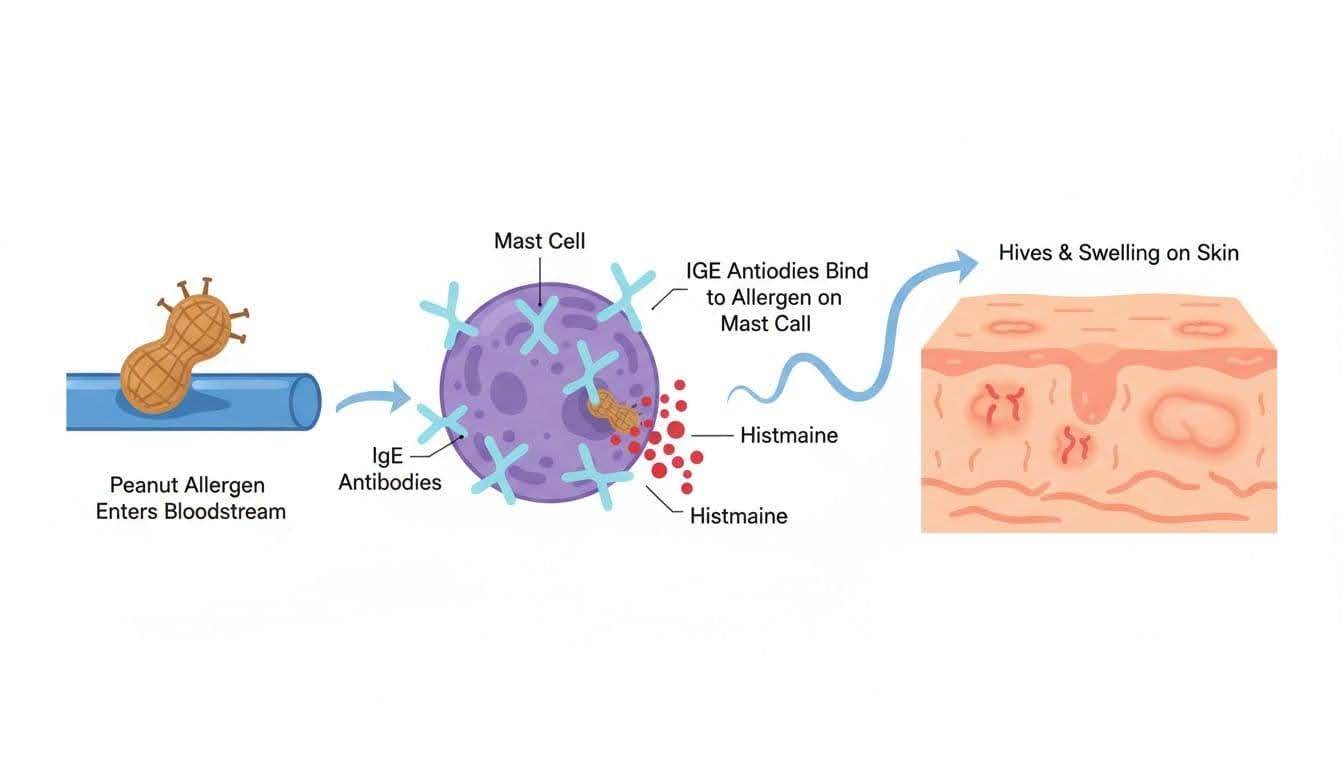
With a true allergy, even a tiny amount can matter. Trace exposure may cause hives, vomiting, swelling, wheezing, or anaphylaxis. Mayo Clinic's explanation of food allergy vs. intolerance makes this point clearly: small exposures can trigger serious reactions.
In the US, the Big 9 allergens cause most reactions: milk, eggs, peanuts, tree nuts, wheat, soy, fish, shellfish, and sesame. Some start in childhood, especially milk and egg allergy. Others appear later. Recent US data suggests nearly half of adults with food allergies developed at least one allergy in adulthood, so this is not only a childhood issue.
What a Food Intolerance Is
Food intolerance usually starts in the digestive system, not the immune system. The clearest example is lactose intolerance. When the body lacks enough lactase, lactose is not broken down well, so gas, bloating, cramps, and diarrhea follow.
Dose often matters here. A little dairy may be fine, while a large milkshake is not. The same pattern can happen with FODMAPs, food additives, histamine-rich foods, or non-celiac gluten sensitivity. Symptoms are real, but the mechanism is different.
Celiac disease sits in its own category. It is an autoimmune disease triggered by gluten, not a classic food allergy, and not a simple intolerance. It needs its own testing and strict management.
Side-by-Side Comparison
The differences become clearer when you compare them side by side:
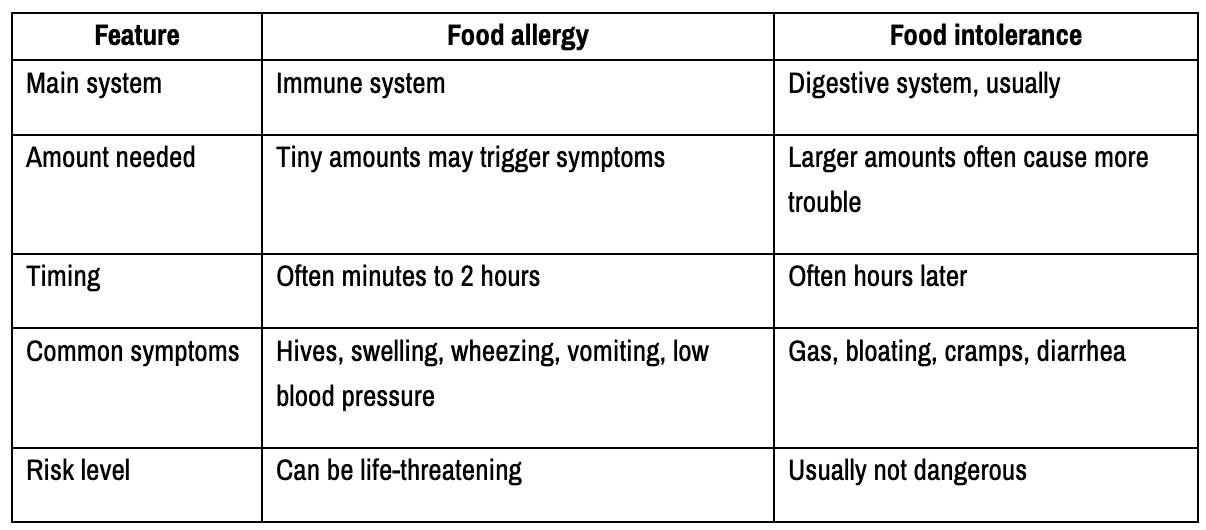
This distinction is even more important when it comes to testing and treatment:
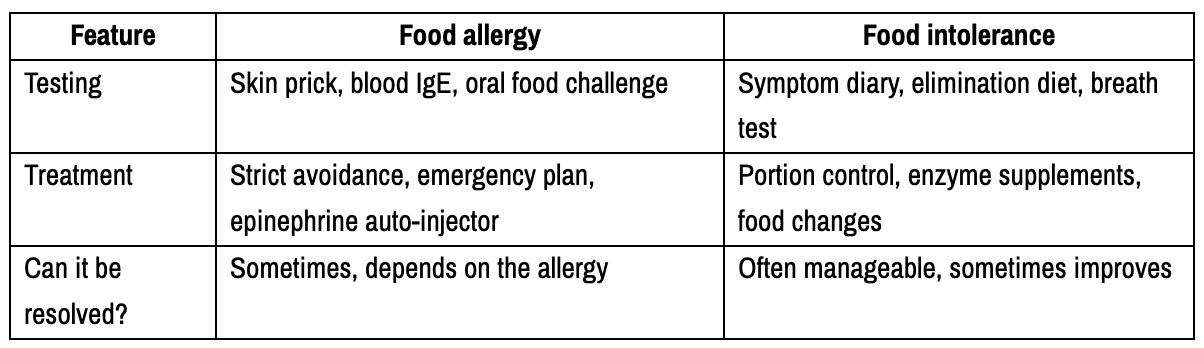
For a plain-language review of how allergists diagnose and treat true allergies, see the AAAAI food allergy overview.
How Symptoms Look, and Why People Get Confused
Allergy symptoms often show up fast and can affect the skin, gut, airway, and blood pressure. Intolerance symptoms usually build more slowly and stay in the gut. That sounds simple, but there is overlap. Vomiting and diarrhea can happen in both, which is why people often mislabel one as the other.
Oral allergy syndrome adds another twist. Pollen-sensitive people may experience mouth itching or tingling when eating raw fruits or vegetables due to cross-reactive proteins. It is often mild and local, but it can be mistaken for a more serious food allergy.
Get urgent care after eating if you develop trouble breathing, throat tightness, faintness, widespread hives, or swelling of the lips or tongue.
The Pairs People Mix Up Most
- Lactose intolerance vs. milk allergy: these are completely different. One is having trouble digesting milk sugar. The other is an immune reaction to milk protein.
- Gluten sensitivity vs. wheat allergy vs. celiac disease: these are three separate problems. A wheat allergy is immune-based. Celiac is autoimmune. Gluten sensitivity does not follow either pattern.
- Histamine intolerance vs. fish or shellfish allergy: flushing, headache, stomach upset, and fast symptoms can look similar, but the cause may be very different.
- IBS vs. food intolerance vs. food allergy: when the gut is the main issue, food is not always the root cause. IBS can react to stress, meal size, gut-brain signaling, and certain carbs.
Getting the Right Diagnosis, and Living with It Safely
Self-diagnosis often leads people astray. Some cut out major food groups that they do not need to avoid. Others miss a real allergy and keep taking risks. Current US estimates put the number of people with food allergies around 22 million, and about 200,000 ER visits happen each year, so getting this right matters.
A food allergy workup starts with the story:
- What you ate
- How fast do symptoms start
- What body systems were involved
- Whether the reaction happened again
Only then do skin or blood tests help. Sometimes an allergist confirms the answer with a supervised oral food challenge. Testing should support the history, not replace it. The AAFP review on food allergy diagnosis and treatment explains why false positives can mislead people.
For intolerance, the workup often uses the following:
- A food and symptom diary
- Brief elimination
- Re-challenge
- Sometimes breath testing
Daily management is different, too. Allergy care focuses on label reading, avoiding cross-contact in kitchens and restaurants, and carrying epinephrine. Intolerance care focuses on portion size, food prep, lactase or other enzyme support, and targeted diet changes.
If symptoms are complex, repeated, or severe, primary care may start the process, but specialist input helps. That is especially true for multiple food reactions, past anaphylaxis, asthma plus food allergy, chronic hives or eczema, and suspected celiac disease. Dr. Grandon's allergy and immunology services are built for that kind of careful evaluation, with telehealth options and a physician perspective shaped by 23+ years of experience.
Key Takeaways
- A food allergy involves your immune system and can become life-threatening. A food intolerance usually involves digestion and is uncomfortable but not dangerous. That one difference changes your testing, treatment, and the level of strictness your daily food rules need to be.
- Symptoms can look similar — which is exactly why self-diagnosis goes wrong. Vomiting and diarrhea happen with both. Guessing can mean cutting out foods you don't need to or staying at risk because a real allergy went unidentified.
- The right diagnosis makes daily life significantly easier. Once you know whether you're dealing with an allergy or an intolerance, the guesswork stops; and so does unnecessary food restriction or unrecognized risk.
⚠️ When to seek urgent care: Throat tightness, trouble breathing, faintness, or widespread hives after eating are emergencies. Do not wait to see if symptoms improve.
What Is Next for You
If you are dealing with repeated food reactions, the goal is not to keep guessing or unnecessarily eliminate foods; it is to get the diagnosis right. Start by noting what you ate, how quickly symptoms started, and what symptoms occurred. This information is often more valuable than testing alone.
From there, a structured evaluation can determine whether this is a true allergy, an intolerance, or another condition entirely.
If you are looking for a more personalized, root-cause approach to food reactions and allergy care, you can join the waitlist for upcoming telehealth consultations.
🔔 Be the First to Know: If you are looking for a more personalized, root-cause approach to food reactions and allergy care, you can join the waitlist for upcoming telehealth consultations. 👉 Join now.
Stay connected with news and updates!
Join our mailing list to receive the latest news and updates from our team.
Don't worry, your information will not be shared.
We hate SPAM. We will never sell your information, for any reason.
